Hello Everyone,
Since my last post was a basic discussion about typical preventative medicine, I thought a good topic for this week would be Lp(a). In conversation, you would call this “Lp little a”. Lp(a) is a lipoprotein similar to LDL. Last week I mentioned that at an annual checkup typically your “cholesterol” would be checked. This usually includes total cholesterol, triglycerides, low-density lipoprotein (LDL -C), high-density lipoprotein (HDL-C), and very low-density lipoprotein (vLDL-C). I’m not going to get into significant detail on what these levels mean today. That will be for another post. However, everyone should know there are much better tests that can be done to identify your risk. The problem is, most insurances do not always cover all of these.
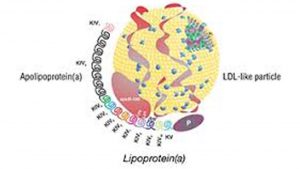
What is important to understand is that an LDL is actually not cholesterol. LDL is a vehicle to carry cholesterol in the blood. Cholesterol is not able to float in the blood without being protected. Lp(a) is basically an LDL with a specific protein “tale”. About 10 to 20% of the population has an increase in Lp(a). This is associated with an increased risk of cardiovascular disease including stroke and heart attack, aortic stenosis, and deep venous thrombosis.
Unfortunately, diet and exercise do not seem to reduce Lp(a). Many of the people who have an elevated Lp(a) will have good cholesterol levels and really no other cardiovascular risk factors other than a family history of early heart disease. If any of you have watched The Biggest Loser you will likely remember Bob Harper. He had a heart attack at the age of 52. All of his cholesterol markers that were checked prior to his heart attack had been normal, he was in great shape and ate well. His Lp(a) was found to be significantly elevated after his heart attack, but he had never had this checked. You may see him on a commercial for a new blood thinner, which I find funny. He should be on TV talking about Lp(a), but I’m sure he is getting paid pretty well from the drug company. Rather than treatment for a heart attack, we should be talking about prevention.
I do not want to get over technical on how this leads to increase risk, but I just want to make our patients aware that it can be a problem and is not something that is often screened for or even fully understood by most providers. You can always ask me further about this if I see you as a patient. Otherwise, I would recommend you ask your provider to have this checked if you are concerned about your risk. Especially if you have a strong family history of cardiovascular disease.
Eric Greene, APRN